Peptide Therapy Myths Debunked: What Patients Get Wrong

Peptide therapy sits at an awkward intersection of cutting-edge science, aggressive online marketing, regulatory confusion, and genuine clinical promise. That combination produces a lot of misinformation. Patients arriving at their first consultation often carry beliefs picked up from Reddit threads, fitness influencers, or half-read news articles — some of which are harmless misunderstandings, and some of which lead people toward real harm. Here are the most common myths, set straight.
Myth 1: Peptides Are the Same as Steroids
This is one of the most persistent misconceptions, particularly in fitness and bodybuilding communities where peptides and anabolic steroids sometimes appear in the same conversations.
Anabolic steroids are synthetic derivatives of testosterone. They work by binding directly to androgen receptors and driving muscle growth, but they also suppress the body's natural hormone production and carry a well-documented list of serious side effects including cardiovascular damage, liver toxicity, hormonal disruption, and psychological effects.
Peptides are short chains of amino acids, the same building blocks as proteins. The therapeutic peptides used in clinical settings — ipamorelin, BPC-157, thymosin alpha-1, GHK-Cu — work through entirely different mechanisms. Growth hormone secretagogues like ipamorelin stimulate the pituitary gland to release your own growth hormone within its natural range, rather than introducing a synthetic hormone from outside. BPC-157 influences growth factor signaling and angiogenesis. Thymosin alpha-1 modulates immune function.
The category overlap that causes confusion: some performance-enhancing compounds used in sports doping, like certain growth hormone secretagogues, are peptides. But the peptides used in clinical medicine are a very different application of the same molecular category. Calling all peptides "steroids" is like calling all proteins "fat" because both are macronutrients.
Myth 2: All Peptides Are Illegal
This was closer to true in the United States between 2023 and early 2026, when the FDA moved many therapeutic peptides to Category 2, effectively cutting off compounding access. During that period, there was no legal clinical pathway for many of the most commonly discussed compounds.
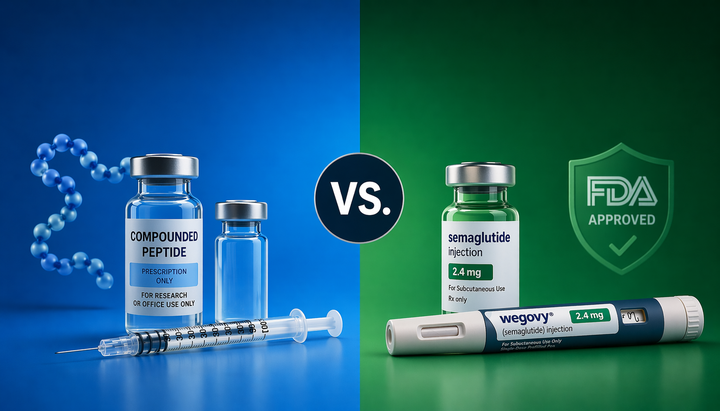
As of 2026, that has changed. Fourteen peptides were reclassified back to Category 1 under Section 503A, restoring the legal pathway for licensed providers to prescribe them as compounded medications. Compounds including BPC-157, ipamorelin, CJC-1295, thymosin alpha-1, and GHK-Cu are now legal to prescribe and dispense through licensed 503A compounding pharmacies.
Additionally, several peptide therapies are fully FDA-approved: semaglutide, tirzepatide, tesamorelin, and liraglutide all have approved indications and are available through standard pharmacies with a prescription.
Peptides accessed outside the licensed clinical pathway — from vendors selling "research use only" products without prescriptions — exist in a different legal category and carry documented safety risks. But the claim that peptide therapy as a category is illegal is simply not accurate in 2026.
Myth 3: You Can Self-Prescribe and Self-Administer Safely
The internet has made it easy to find peptide dosing protocols, purchase compounds without a prescription, and manage a self-directed therapy program without any provider involvement. Many people do this. It does not mean it is safe.
The risks of self-directed peptide use cluster around several specific problems. First, without a clinical assessment, there is no way to screen for contraindications. Growth hormone secretagogues are not appropriate for people with active or history of hormone-sensitive cancers — a fact a provider would catch; a Reddit post would not. Second, without lab monitoring, there is no way to detect adverse changes in IGF-1 levels, blood glucose, or other markers that would prompt dose adjustment or discontinuation. Third, without a licensed pharmacy, there is no quality control on what you're actually injecting.
The clinical pathway exists not as bureaucratic friction but because these compounds are biologically active and individual responses vary. Appropriate oversight materially reduces the risk.
Myth 4: More Peptides and Higher Doses Produce Better Results
The appeal of stacking multiple peptides and escalating doses is understandable — if one peptide supports recovery, surely three will do it faster. This logic does not hold in practice.
Most therapeutic peptides operate through receptor-mediated mechanisms with a ceiling effect. Beyond a certain dose, additional compound does not produce additional benefit and may increase side effects or provoke receptor desensitization. For growth hormone secretagogues in particular, the pituitary's response to stimulation is limited by feedback mechanisms. Stacking ipamorelin with CJC-1295 has a rational basis in combining different half-lives; stacking five growth hormone secretagogues at maximum doses does not.
More broadly, the interaction effects between multiple peptides are poorly understood. There are almost no human studies examining peptide combinations, and the preclinical data is limited. A responsible clinical protocol uses the minimum effective dose to achieve a defined goal, monitors for response, and adjusts from there.
Myth 5: Peptide Therapy Is a Quick Fix
Therapeutic peptides are not acute interventions. They work through biological processes that operate on timescales of weeks to months. Growth hormone secretagogues, for example, produce effects on body composition and recovery through gradual changes in growth hormone pulsatility and downstream IGF-1 activity. BPC-157's tissue repair effects, where they occur, emerge over weeks of treatment.
Patients who expect dramatic results within days are likely to be disappointed and may be tempted to escalate doses or switch compounds prematurely. The appropriate approach is a defined protocol with clear outcome measures, monitored over a clinically relevant timeframe, with provider check-ins to assess response.
Myth 6: If It's Natural, It Must Be Safe
Several therapeutic peptides are derived from or structurally related to naturally occurring proteins. BPC-157 is isolated from a sequence found in human gastric juice. Thymosin alpha-1 is a hormone produced by the thymus. GHK-Cu is found in human plasma.
"Natural" is not a proxy for safe. Many natural compounds are toxic at certain doses or in certain contexts. The relevant question for any therapeutic agent is not whether it occurs naturally but what the evidence shows about its safety profile at therapeutic doses in the relevant population — and what is known about interactions with existing health conditions and medications.
The natural origin of some peptides is scientifically interesting and may contribute to favorable tolerability profiles, but it is not a basis for assuming safety or skipping clinical oversight.
Myth 7: Peptide Therapy Is Only for Athletes and Bodybuilders
The dominant online discourse around peptides does skew toward athletic performance and physique goals, which has shaped public perception. But the clinical applications of peptide therapy extend well beyond that population.
Thymosin alpha-1 is studied for immune support in aging and in patients with impaired immune function. Larazotide has been in clinical trials for celiac disease. Selank and semax have been investigated for anxiety and cognitive support. GHK-Cu is used in dermatology contexts for skin regeneration. GLP-1 peptides are the most-prescribed weight management medications in history. The patient population interested in these therapies is diverse — older adults interested in healthy aging, people managing chronic conditions, patients looking for recovery support after surgery or injury.
The bodybuilding association is real but represents one slice of a much broader clinical picture.
Frequently Asked Questions
Are peptides the same as hormones?
Some peptides act as hormones — GLP-1, for example, is a naturally occurring hormone, and GHK-Cu is found in plasma. Others, like BPC-157, are not classified as hormones. Growth hormone secretagogues stimulate hormone release but are not hormones themselves. The category of "peptide" describes a molecular structure (short amino acid chains), not a function.
Do peptides show up on drug tests?
Some peptides are banned by organizations like WADA (World Anti-Doping Agency) for performance enhancement. BPC-157 was temporarily on WADA's list, though it is not currently prohibited. Any athlete subject to drug testing should verify the current status of a specific compound with their relevant governing body before use.
Can peptides reverse aging?
No peptide has been shown to reverse aging in humans. Several compounds, including epithalon and MOTS-c, are being studied for effects on aging-related biological processes, and longevity science is an active area of research. The honest characterization is that some peptides may support processes associated with healthy aging, not that they reverse the aging process.
Do I need to inject peptides, or are there oral options?
Delivery method depends on the compound. Some peptides can be administered orally or nasally, though oral bioavailability is often lower than injected forms because peptides are broken down in the digestive tract. Injectable administration is the most common route for most therapeutic peptides currently prescribed in clinical settings. Oral semaglutide (Rybelsus, Wegovy oral) is one of the few exceptions with established oral efficacy.
Is peptide therapy approved by mainstream medicine?
FDA-approved peptide therapies (semaglutide, tirzepatide, tesamorelin) are fully within mainstream medicine. Compounded peptides prescribed through licensed providers exist at the intersection of conventional and integrative medicine. The clinical community's view of individual compounds varies — some have broader mainstream acceptance than others. A provider's role is to help you understand where the evidence stands for a specific compound relative to your situation.
Sources
- Józwiak M, et al. Multifunctionality and Possible Medical Application of the BPC 157 Peptide. *Pharmaceuticals (Basel).* 2025;18(2):185.
- Vasireddi N, et al. Emerging Use of BPC-157 in Orthopaedic Sports Medicine: A Systematic Review. *HSS Journal.* 2025.
- Lim M, et al. Weight Loss With GLP-1 Agonists in Nondiabetic Adults: Systematic Review and Network Meta-Analysis. *Obesity.* 2026.
- U.S. Food & Drug Administration. FDA-Approved Drug Products. FDA.gov
- World Anti-Doping Agency. Prohibited List. WADA-AMA.org
This content is for educational purposes only and does not constitute medical advice. Peptide therapies should only be pursued under the supervision of a licensed healthcare provider. Amino Clinic recommends consulting with your physician before starting any new therapy.